Advertisements
Do you have melanoma? Are you worried about a mole on your back? Read this article and find out what melanoma is, how it is diagnosed and cured.
Its full name (malignant melanoma) might fill you with dread. But if you are not a physician, you will have little clue of what this disease is exactly. Here is some help to understand, identify a melanoma, so you will know what to expect from your MD.
Related Topics (Ads):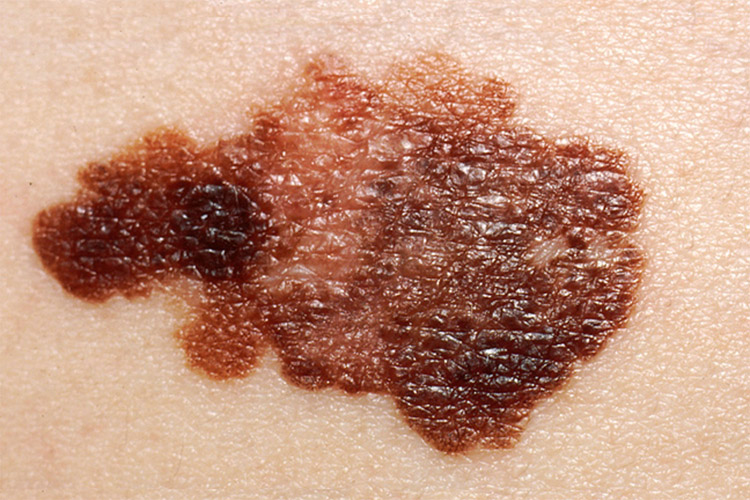
What is melanoma?
Melanoma is a type of skin cancer developing from melanocytes. These cells are the ones producing melanin, the pigment in your skin. This pigment is responsible for your complexion, for the color of your hair or eyes, for the red in your lips, or even for tanning in summer.
A very common and dangerous form of cancer
In the case of melanoma, melanocytes start multiplying uncontrollably and turn into skin cancer.
You should know melanoma is the most dangerous type of skin cancer. Its fast development, ability to create metastases (developing in other regions of your body) easily or to be mistaken for a common mole makes it one of the most dangerous and insidious among cancers and a real threat to public health.
How do you get melanoma?
What are UV rays and what role do they have?
The main cause behind this dreaded disease is UV radiation. UVs are a specific type of sun rays (making up 10% of natural sunlight), which are deadly to humans. While some of these rays are stopped by ozone in the atmosphere, some others will reach the beach where you have set down your towel anyway.
As mentioned earlier, UV rays are naturally present in sunlight, but you can also find them in:
- Sunbeds
- UV lights
- Lasers
- Luminotherapy lights
- Insect traps
Of course, among those, the most dangerous would be sunbeds. You lie down, hoping to work on your complexion and get a nice suntan to show your friends at the beach but overusing them might cause you to develop skin cancer.
But UVs are not all that bad, are they?
No, they are not: you actually need them to produce vitamin D, a vitamin necessary to absorb calcium, magnesium, or phosphates, all of them essential to life. But you should know exposing your body 15 minutes two or three times a week is enough to produce the quantities you need, according to World Health Organization recommendations.
UVs are also beneficial to some skin conditions like psoriasis, eczema, jaundice or vitiligo.
So, get a bit of sunlight in your life, but do not abuse it!
Genetic mutations
Although UV rays are behind your wonderful tan in summer and the simple but painful sunburns when you stayed on the beach just a bit too long, they can also cause genetic mutation in the skin by damaging DNA, which can lead to melanocytes multiplying without control and therefore melanoma.
Overexposure to sunlight being the major risk factor leading to melanoma, the disease mostly appears on frequently exposed areas of the body:
- Back (especially for men)
- Shoulders
- Legs (especially for women)
- Arms (forearms, mostly)
How is melanoma diagnosed?
What will your doctor look for?
Quite simply, doctors have a mnemonic to identify melanomas and differentiate them from common moles:
- Asymmetry: moles are usually symmetrical, whereas melanomas are not
- Borders: moles tend to form nice round shapes, while melanomas are irregular and form corners and edges
- Color: melanomas exhibit different colors and hues
- Diameter: melanomas often exceed 0.24 in (6 mm) in size
- Evolution: melanomas evolve, continue to grow and change shape
- Funny looking: moles are usually round and consistent in color, whereas melanomas are different, quickly looking like something that should not be there
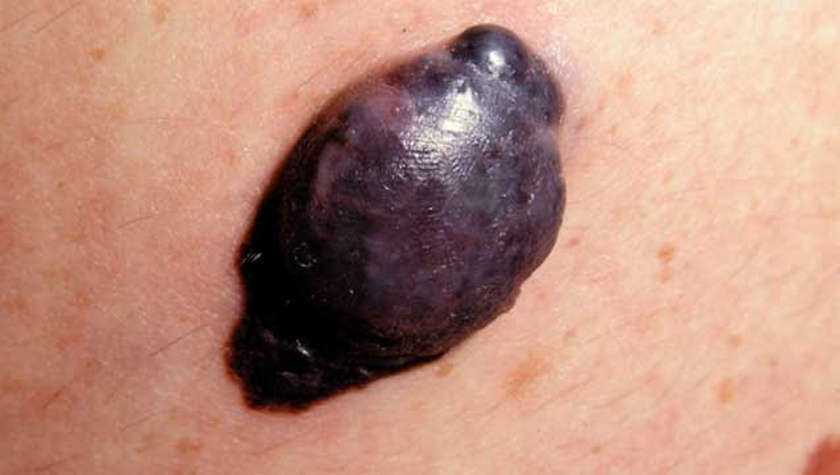
Nodular melanoma: a more aggressive form of melanoma
The most aggressive form of melanoma (nodular melanoma) has other symptoms, therefore another mnemonic:
- Elevated: nodular melanomas form above the skin and consequently appear like they are growing “out” of the skin
- Firm to the touch: nodular melanomas are hard
- Growing: as mentioned above, this form of melanoma is extremely aggressive, meaning it grows extremely fast
Confirming the diagnosis
Generally, your MD will also try to compare what he suspects to be a melanoma with other skin lesions like common moles or keratosis.
But since there are different types (4 main types but over 10 in total) of melanoma, a biopsy will always be necessary to confirm the diagnosis: your doctor will cut out a small piece of the suspicious mole and send it for analysis to a histologist (an MD specialized in analyzing tissue samples).
You should also note it is not uncommon for doctors to take pictures of your entire body to:
- identify other potential sites on which melanomas could have developed
- have a base photography for follow-up consultations and study the evolution of the disease
What about treatment?
Surgery is always the first-line treatment
As a biopsy is always required to confirm the diagnosis, a patient suspected to suffer from melanoma will have to go under the knife.
After taking the sample, your surgeon will usually immediately continue the procedure (or schedule a later one) with wider excision of the lesion. This means that your surgeon will not only cut out the mole suspected to be a melanoma, but also a small patch of clear skin around it, just to be safe.
In the case of melanoma, it is very frequent to undergo multiple surgeries so as to avoid recurrence (the risk of having the disease grow back).
Complementary treatments
Called adjuvant treatments, these try to complete surgery and reduce the chance of recurrence.
Your doctors can use a wide range of adjuvant treatments, like:
- Interferon is frequently prescribed in the USA, but not in the UK or other European countries since doctors there consider this treatment to have too few benefits and too many side effects.
- Chemotherapy is also frequent (particularly in the US) and dacarbazine is the chemotherapy drug of choice in this case.
- Targeted therapy consists of using a molecule to slow down the evolution of the disease and the multiplication of tumorous cells.
- Immunotherapy is a bit similar but calls upon your own antibodies and leukocytes (white blood cells) to destroy the tumor.
- Radiation therapy also often complements surgery, particularly if the cancer is located in a hard to reach area.
Conclusion
A suspicious mole is not necessarily a melanoma and the sooner your doctor identifies a melanoma, the more efficient the treatment will be.
So if you have any doubt, do not hesitate and consult an MD.
Related Topics (Ads):References:
Melanoma Warning Signs – What You Need to Know About Early Detection 2. What to Know About Melanoma 3. Melanoma: Introduction to a Deadly Skin Cancer 4. What Causes Melanoma Skin Cancer? 5. Melanoma Risk Factors 6. Risk factors for melanoma 7. Medical Definition of Melanoma, benign 8. Mole or Melanoma? Tell-Tale Signs in Benign Nevi and Malignant Melanoma 9. Four Main Types of Melanoma 10. I’ve Been Diagnosed with Melanoma. Now What? 11. Tests for Melanoma Skin Cancer
Advertisements
